by Dr. Shapira | Jul 29, 2021 | Muscular Skeletal Dentist, MUSCULOSKELETAL DENTISTRY, TMJ Chicago
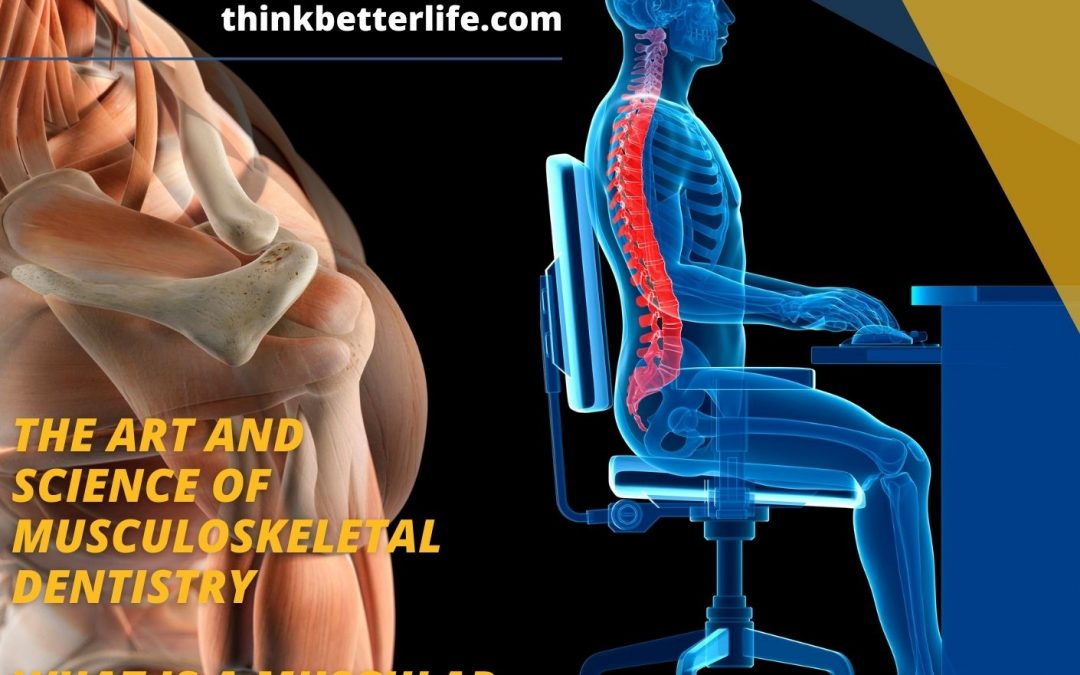
Myofascial Pain and Dysfunction the most common cause of pain is best addressed utilizing Musculoskeletal Dentistry to correct functional and physiologic issues that can cause TMJ Disorders (TMD), Headaches, Migraines, Neck and Shoulder Pain, Forward Head Posture and...
by Dr. Shapira | Oct 24, 2020 | Blog, TMJ Chicago
This is a video on the development of TMJ Disorders and Sleep Apnea. While my practice is generally adult oriented for treating Orofacial Pain, TMJ Disorders and Sleep Apnea the prevention of these problems in children is of utmost importance. This video is one made...
by Dr. Shapira | Jul 1, 2018 | Blog, Chicago, Highland Park, Lake Bluff, Lake Forest, Libertyville, TMJ, TMJ Chicago
Chronic Sinus Headache and other Sinus Pains are closely related to TMJ Disorders. The connections between these problems is multifacted. The Trigeminal Nerve also called the Dentist’s Nerve is the underlying common source of all of these problems. Dentists are...

by Dr. Shapira | Aug 13, 2017 | Always tired cause by lack of sleep, Blog, Blog migraine, Causes of TMJ, Clicking & Popping, Diagnosis of TMJ, SPG Block Anxiety, SPG Block Cluster Headache, SPG Block Migraine, SPG blocks, Sphenopalatine Ganglion Blocks, TMJ, TMJ - General, TMJ affects your posture, TMJ ARTHRITIS, TMJ Chicago, TMJ CREPITUS, TMJ Neck & Back Pain, TMJ Specialist, Treatment of TMJ, Trigeminal Nerve, Trigeminal Nervous System, Trigeminal Vascular System, Unsorted
The number of abbreviations in medicine and dentistry is amazing. In this short post I am going to give only a small number of definitions routinely utilized in literature and culture concerning TMJ disorders, often called “the Geat Imposter” This will...
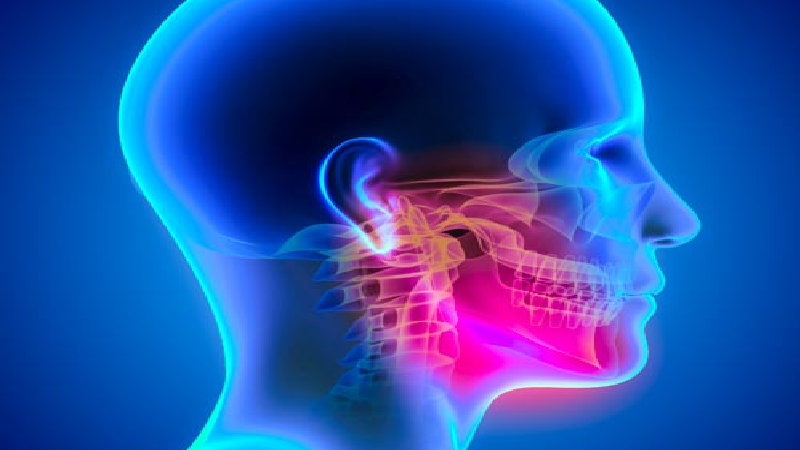
by Dr. Shapira | Feb 29, 2016 | antidepressants sleep apnea, Anxiety, autonomic cephalgias, BARRINGTONOROFACIAL PAIN KENOSHA OROFACIAL PAIN, Blog, Breathing Sleeping Problems, Causes of TMJ, Chicago, Chronic Daily Headache, Cluster Headache, Crowns & Bridges, Depression and Chronic Pain, Depression and Sleep Disorder, Diagnosis of TMJ, Jaw Pain, Jaw Problems, Medication for TMJ, orofacial pain, SPG Block Anxiety, SPG Block Cluster Headache, SPG Block Migraine, SPG blocks, Sphenopalatine Ganglion Blocks, tension Headache, Throat & Swallowing TMJ, TMJ, TMJ - General, TMJ and sleep disorders, TMJ Chicago, TMJ is a painful condition, TMJ Specialist, TMJ SUBLUXATION, Trigeminal Autonomic Cephalgias, Trigeminal Cervico-Complex, Trigeminal Nerve, Trigeminal Nervous System, Trigeminal Vascular System, Trouble breathing while asleep
Orofacial Pain Referral: https://thinkbetterlife.com/referrals/ View patient video testimonials: https://www.youtube.com/channel/UCk9Bfz6pklC7_UluWFHzLrg/videos What is Orofacial Pain and how does it relate to TMJ Disorders and Headaches. Please visit this entire...





